We had a really scary time this week — my 11-year-old son ended up in the Pediatric ICU at the local children’s hospital for two days due to Diabetic Ketoacidosis and we found out he has Type 1 Diabetes. I’m sharing our story because I missed obvious signs. Maybe another parent or caregiver might miss signs too. Maybe this will save a kid from going into Diabetic Ketoacidosis. While Type 1 Diabetes is not curable; maybe if I had put things together, we could have prevented a 2 day stay in the Pediatric Intensive Care unit. Our Diabetes Story: My 11 year old went into DKA and was diagnosed with Type 1 Diabetes | The Mama Maven Blog Our Diabetes Story: My 11 Year old Son Went Into Diabetic Ketoacidosis and Has Type 1 Diabetes

According to the Juvenile Diabetes Research Foundation: “Knowing the warning signs for type 1 diabetes could help save a life! Type 1 diabetes can often go undiagnosed in its early stages because the symptoms can be mistaken for more common illnesses, like the flu. Take notice if you or your loved one experiences the following:
- Extreme thirst
- Frequent urination
- Drowsiness and lethargy
- Sugar in urine
- Sudden vision changes
- Increased appetite
- Sudden weight loss
- Fruity, sweet, or wine-like odor on breath
- Heavy, labored breathing
- Stupor or unconsciousness
Call your doctor immediately if one or more of these symptoms occurs in you or your loved one. It is extremely important to receive medical attention—misdiagnosis or leaving your condition untreated can have tragic consequences, including death.”
This is how we wound up at the hospital:
Last Friday night B vomited (food) late at night. I didn’t think anything of it because he had eaten ice cream with his cousins and then miso soup and samosas for dinner. Crazy combination, right? He was fine all weekend after that and I was watching him closely. He seemed tired and very thirsty. (WARNING SIGNS). However, it was a hot, late August weekend and I ran my kids around a lot running errands and having plans. My husband was out of town on a trip in Bulgaria and we were on stay cation at home and having a grand old time. On Monday, we didn’t RSVP for the Eclipse activities at the Queens Library Forest Hills and were told we wouldn’t get in, so we ran home quickly (in the heat) to watch the eclipse. B insisted on carrying his own water and this set off something in my head because he was really drinking alot (WARNING SIGN ). Later that night, B told me he didn’t want to eat dinner and I let him skip it (turns out later he ate 1/2 a small package of candy without me seeing). My husband came home that night and all was well in our world.
The Catalyst:
Then, at 3:30 in the morning, B starting throwing up. He threw up water (yes, we always check) and since he had just been sick, we figured it was gastro-related. I was tired and went back to bed, but my husband stayed up with him for a while since he had jet lag anyway. B kept throwing up and throwing up. He kept trying to drink water. When I got up with him, early in the morning, I tried to regulate what he was drinking. I figured that he would be okay if he rested and stopped drinking. I figured wrong. He tried to make his own energy drink with juice, water and honey and threw that up too. He was supposed to go on a trip with my in-law’s at noon that day. But around 9AM, I looked at B and he just looked gray and sunken (WARNING SIGN). So pale and so skeletal. He’s a skinny kid as it is, but something was off.
I realized that we needed to go see the doctor right away. I called our pediatrician’s office and told them he couldn’t stop vomiting and he needed to come in NOW. They told me to come in at 11:15. That’s what they always say and I always ignore them and show up anyway. I quickly showered for a hot second and yelled at everyone to get ready to leave. So, of course, his little brother, S, did nothing. He’s 7 and not the easiest kid. I finally got him to get dressed about 5 minutes later and then had to put on 3 shirts before he would accept one. I packed my things and things for my kids, I had a feeling we were going to be at the doctor’s office for a while.
B was lying on the floor at this point. He told me he was having trouble breathing, which really confused me. S took his time putting his shoes on — we couldn’t wait anymore so I put them on and he freaked out. At that point, we couldn’t wait and somehow I got him to leave without the usual screaming tantrum. My daughter grabbed his hand and led him to the subway and I helped Ben. I had a bucket in a tote bag in case he threw up. I was thinking about calling an Uber, but knew the subway was going to get us there faster (our doctor is two stops away on the F train or one on the E train). I thought the doctor’s office would give him Zofran to stop the vomiting and he’d be okay. With my ulcers, I’ve vomited a lot and I figured it was stomach related due to the vomiting three nights before. Once we got to the pediatrician’s office, our doctor heard us come in and brought us water immediately. B guzzled it down. The doctor looked at him and said it was either gastro-related or something else. “Something else? What?”, I thought. The doctor asked me to help my kid pee in a cup. I helped B to pee and figured we’d get that Zofran and be on our way.
Answers?
The urine was tested and the glucose was 500 – which was dangerously high and my son had ketones of 160 mg. Now, I really didn’t understand that he was in Diabetic Ketoacidosis (called DKA), but it’s really bad. As he could have gone into a coma and possibly died kind of bad.

I had Gestational Diabetes with my last pregnancy in 2010 and I don’t remember glucose levels and the lingo. Things started happening fast here. Luckily while this was all going on, the office was quiet and my two younger ones were quiet and engaged with the iPad (usually my little guy would be carrying on). The doctor told us we needed to go to the Emergency Room. The word diabetes was mentioned. I was still pretty confused at this point. I tried to keep it together though. The doctor called an ambulance and I asked to be taken to Cohen’s Children’s Hospital – we’ve been there before and they’ve always treated us wonderfully. And from the R Baby Foundation, I knew that a children’s ER was a better place for my son to be than a regular hospital. However, another hospital’s ambulance was there and they said they were taking us to their hospital. There was no children’s ER there. I called my sister-in-law, G, who’s a doctor and she called the pediatrician. This part is blurry — but they agreed to take us to Cohen’s Children’s hospital (I’m not sure if they said yes because she was telling for them to do that or if they took us because I kept asking to go to Cohen’s).
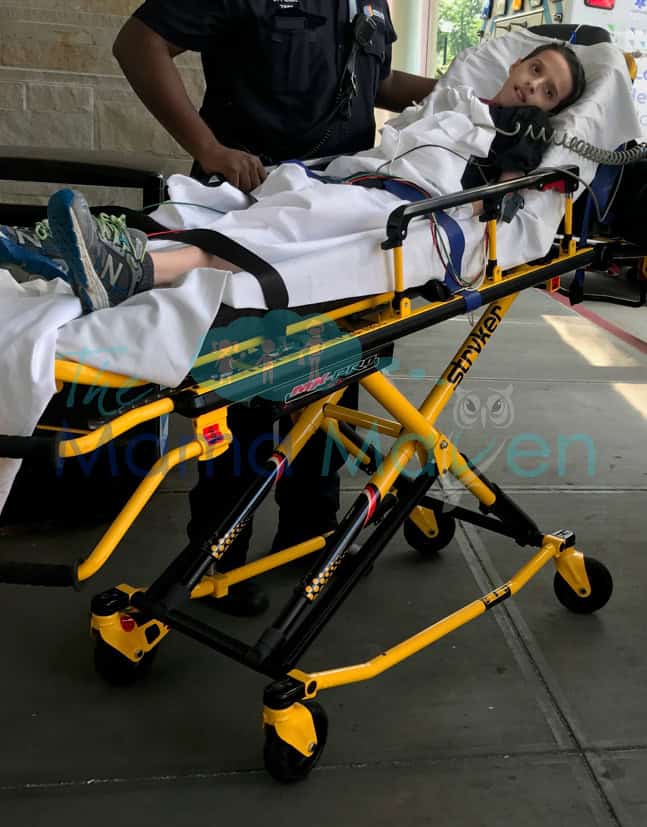
Here is an image of how my son looked after getting fluid in the ambulance. Honestly, it’s hard for me to look at but you can clearly see that something is very, very wrong with him.
Going to the Children’s ER
We went to Cohen’s – S loved the ambulance ride and he was an angel (usually not the case). They started an IV of fluids for dehydration for B in the ambulance. The EMT with us was wonderful and we were at Cohen’s around 20 minutes later – luckily no traffic! At this point, I didn’t know what was going to happen – how could my kid have diabetes? The EMT told us that he thought we were going to be admitted into the hospital to stay. I thought back to when B being recently – and even excessively thirsty over the weekend – it was summer in NYC and it is hot out.
My mother was there already when we got there in the ambulance. My in-laws and my husband showed up quickly. My sister-in-law G came. My mother quickly took my younger son and daughter with her because the ER waiting room is no place for them to hang out and my mother lives nearby. I have no sense of time and I am not sure how long we were in the ER, it could have been 1 or 2 hours. It could have been longer. My mind was spinning and I wanted to vomit myself. But, as a parent, I had to hold it together for my kid.
The staff at Cohen’s started treating B. We had fluids started but they stopped him from drinking water. He looked so pale and sick and my heart was just breaking. The doctor we saw said that he sees at least one child a day who’s in Diabetic Ketoacidosis – which was shocking to me. B was going to have to go up to the Pediatric ICU and we were told he was going to be there for a few days. His white blood cells were elevated (at 25). We weren’t going home. This was bad. We were sent up to the Pediatric ICU (called PICU for short).
Walking through the halls of the PICU was very humbling. Seeing children in beds and cribs, so still was scary. What was happening to my kid was scary. I’ve never seen him like this. I couldn’t wrap my head around Type 1 Diabetes. B kept begging for water and finally they let him have ice chips, but not a lot. Hours later we were still only allowed to give him ice chips. The IVs hurt his arms. My husband, who is an amazing father, was great.
We called my mom to bring the two younger ones back to meet my in-laws’ at the ER so they could take them back to their house upstate. I had to focus on B and if S was around, I couldn’t do that. I wasn’t planning on leaving B at all. My husband was going to go back home for me but I also had to quickly pack up clothes for my younger kids and I just drove home to do that. I came home, cried quickly (frankly, I was a mess!), and my neighbor V and her son came up to help me. Her son helped me find B’s favorite stuffed animal (which I couldn’t find) and pack. I quickly took a shower when my MIL and my daughter walked in. My daughter almost took my suitcase, but I quickly corrected that and I left to go back to the hospital. My mother came to be with us in B’s room and made sure I ate dinner (all I had to eat was a shot of wheatgrass juice in the morning and a granola bar that my sister-in-law G gave me).
I went back to the PICU and settled in for the night. B was able to nap a little. The night nurse came on at 7PM and was terrific. My son started a dose of insulin that night. I sent my husband home around 9 PM to get some rest. The night wasn’t easy, B couldn’t sleep. I let him watch the Disney Channel, but I got a couple of hours sleep and eventually, he got around 2-3 hours.
The next morning he looked much better, but not quite himself. At 9AM he was cleared to eat and I went down the cafeteria to get my boy some french toast. While we knew things were going to change, he was allowed one last meal without counting carbs.
I learned a lot about Type 1 Diabetes on Wednesday — it’s not really about watching sugars in foods. It’s more counting carbs in food and making sure sugars aren’t so high. The social worker came in and the Diabetes Educator came in. I learned more about Type 1 Diabetes than I wanted to. It was intense. He had a carb counted lunch and then a carb counted dinner.
We were taught how to count his carbs and how to check his blood sugar and to give injections of insulin (the day dose 3x a day and the night dose before bedtime). We were allowed to leave right after we took the night dose of Lantus (the longer acting insulin). We left the hospital at 10PM.
The next day (yesterday) we spent the whole day at the Endocrinologist’s office, with the diabetes educator and the dietician. Learning even more about Type 1 Diabetes. Learning how to count carbs and correct blood sugar. We know there is a long road ahead of us and while last night and tonight I ended up calling the doctor because of issues, we are 100% committed to helping him. I admit I am totally overwhelmed and I’ve been crying a fair amount. We haven’t slept very well, but luckily I am eating really cleanly and that has definitely made sure that I’m not going off the rails.
I will be writing updates about our journey and I hope that our experience and the warning signs can help. Unfortunately, this is going to change a lot of things about our daily lives, but we will find our new normal.
Note: I am not a doctor or have medical training. I talk about Type 1 Diabetes from a parent’s point of view. Always consult your endocrinology team if you have any questions. I advocate for my child until he can advocate for himself.
Read our 2 week update: http://www.themamamaven.com/our-diabetes-story-type-1-diabetes-update/

Read out 1 month update: http://www.themamamaven.com/one-month-since-my-sons-type-1-diabetes-diagnosis-and-hospitalization/




About 1 year ago my I went through the exact same scenario with my 11 year old daughter (she was diagnosed at 10) we too missed all the signs she could have died. It’s still hard for me to think about the events and missed signals leading up to being in ICU with blood sugar levels of 611. Thank you for sharing your story. I’m still having difficulties coming to terms with my daughter having this disease for the rest of her life but i praise God everyday that I have her.
Thank you for sharing your story. It took me a long time to begin to forgive myself for not realizing what was happening. I still struggle with it, but I am so glad that my son is so much stronger now.
Thank you for sharing this. My goodness, my 11 year old has just been diagnosed. We also landed up in icu. So much to learn and life and meals as we know, have changed. We are so ready to walk the road with our little man. Thank you, I feel like you have written my story!
Oh Heidi,
I’m so sorry. I’m here for you — please feel free to email me and I’ll help you as much as I can.
Thank you for sharing! I am in your spot today!!! Like you are telling my daughter’s story today. I wish I would have read this earlier .
Oh Mandy, please email me offline and I will try to help you as much as I can. My son is doing so much better now – though we do have many ups and downs. He’s strong and if we can do this, you can do this. themamamaven@gmail.com
I am 11 and I got type 1 diabetes in October 2017 in 3rd grade. We cough the sighs early. My blood sugar was 422 and it was scary at first. I was o lu allowed to ha e ice chips and I accidentally spilled them on the bed. I was only in the hospital for less than day. Now I am in 5th grade I am wise to everything now and I have the dexcom g6 I love it so much.
Hello! I am very motivated after reading your article. Thank you for sharing your knowledge and experience. Diabetescentrale.nl
Thank you for sharing all of this. Holy cow — so much to learn. Sending support your way.
Thanks, Paula.
I can only imagine how but scary this was for you! But thank you for sharing your story, you never know who it might help
Being a mom of a child with type 1 diabetes I feel like it has changed our lives. My husband also has type 1 so now that my child has it I am a better wife. I understand so much more about the autoimmune disease now and can help them both much better. I just wanted to send hugs because every day you have to stay on top of things. I’m a blogger too and I feel that I blog less because I’m trying to stay on top of my daughter’s health needs. Wishing you and your family the best.
Thank you, Elle. I’ll check out your blog!
Thank you so much for sharing your journey! I can only imagine how scary this experience was for you. These are signs that I would have went past me completely but I’m so happy he’s now okay.
Thank you, Adanna!
Thank goodness you trusted your momma instincts to take him to the Dr asap. What a scary situation. I will be following along to see how he is doing. Stay strong!
Thank you, Reesa.
What a story Nancy! Thank God your son was diagnosed in time. Thank you for sharing & I wish you all the best as you make life changes for his health.
Thank you, Denise.
Still sounds like you caught it earlier then we did. We skipped the ambulance ride to the local hospital but our son was intubated and almost taken by care-flight to the local children’s hospital. We stayed almost 4 days due to his condition and 2 days of crash course carb counting and Type 1 insulin trianing. So glad that he is home but I know that rough days are ahead! Things will be crazy. Friends and family will NOT understand. Your son will have days where he feels great while other days he may feel miserable all due to Type 1 Diabetes. You will make it! You will learn and learn and grow together.
Welcome to the club— The D-Mom Club
Thanks Thaleia, I read your whole story and your blog has become a source of information and help for me.
Love you Nancy… thoughts and positive vibes to you and your family
Thank you, Irina.
I am so glad that he is on the road to feeling better and that you were able to receive the care you needed. I am sure that it was a scary experience. Please let me know if you need anything. So glad you shared the warning signs as I did not know them and I’m sure others will benefit from learning them too
I am so glad your son is ok! Thank you so much for sharing your story.
Wow what a crazy story- but how helpful to so many I had a diabetic camper this summer she is 5. It was so crazy but she was 3 years in and had a very normal camp experience with 3 very quick nurse trips a day
Hang in momma sounds like you are doing great
My heart goes out to you my son was diagnosed at the age of 21 months old he is now 32 years old. One important thing is to make sure they test him for Celiac’s disease. The children’s hospital here didn’t check him till he was 19 and we found out he had it. Many kids do and cant eat gluten I hope they did check for it most hospitals do now. It effects there blood sugars because of the way they are effected by gluten. We have a pump with an alarm he just decided to do that this past year. I know there is so much information online to help new parents with it now. Make sure they are insulin and Glucagon trained at school . I had a lawyer to help me make sure our schools here in California followed my IEP we had for him for other health impaired. Our school had 6 people always on site trained to give these items. I made sure he didnt hang out where the sick kids were in the nurses office either to do his insulin and blood check. Many things the school back then tried to force me to do but I hope where your at they have had experience with it and are on board to help him. We did not let them test him if he had a low BS it can effect his test scores too. Lots of info out there to learn about but with the internet I’m sure you can get many of your questions answered. They have advocacy groups that can help too if you have any school issues.
Thank you, Laurie.
Wow! I can’t imagine what you must have been feeling and are still feeling. I’m so glad that you were able to get medical help for B in time.
Thank you for sharing the warning signs. I’ll definitely share them with family and friends too.
Thank you, Jillian.